Surgical Correction of Distal Radius Malunions Using an Anatomic Radial Locking Plate
Miguel A. Pirela-Cruz, M.D., F.A.C.S.
Professor & Chairman, Texas Tech University HSC
Paul L. Foster School of Medicine, El Paso, Texas
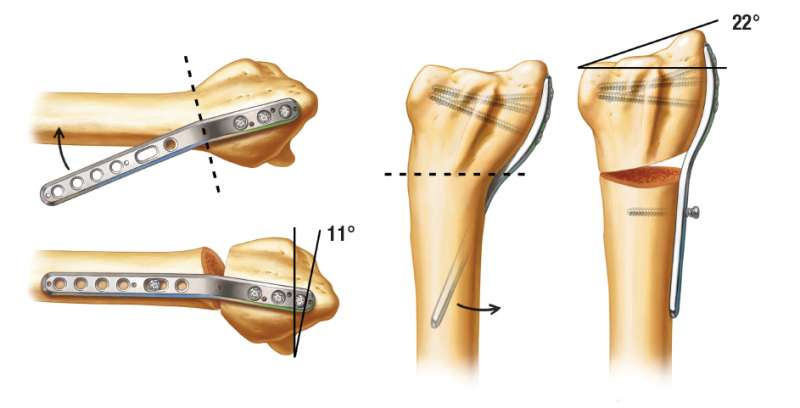
Extra-articular malunions of the distal radius can be corrected using the TriMed Malunion Plate. The Malunion Plate acts as a template for the correction. It provides 11 degrees of palmar tilt and 22 degrees of radial inclination.
Indications:
1. Minimal intra-articular deformity.
2. Minimal arthritis.
3. Good bone stock.
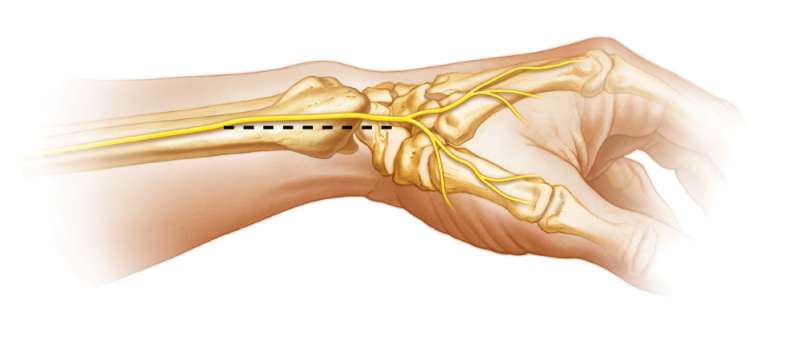
Skin Incision
A direct radial approach is used with a linear skin incision made along the mid-axis of the forearm at the level of the wrist on the radial side.
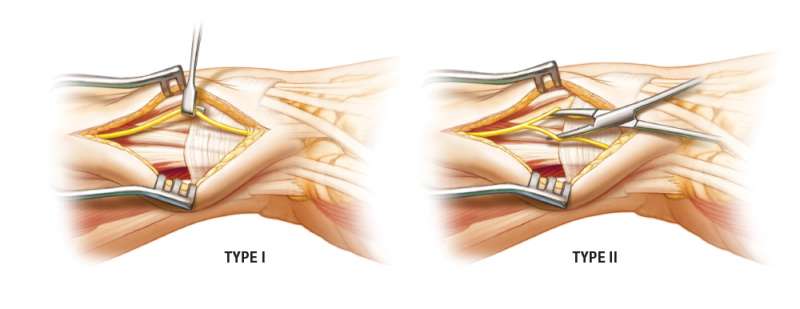
Mobilization of the SBRN
One of two patterns of the Superficial Branch of the Radial Nerve (SBRN) is usually encountered:
A Type I pattern occurs when the SBRN is a single unit that can be mobilized either dorsally or palmarly. A Type II pattern occurs when the SBRN splits into two large branches. The Type II pattern requires careful intraneural dissection to separate these branches for mobilization out of harms way.
Tendon Release of First Dorsal Extensor Compartment
An extensive release of the tendons of the 1st dorsal extensor compartment is performed. If the Extensor Pollicis Brevis (EPB) tendon is found in a separate compartment as may occur, this tendon also requires release.
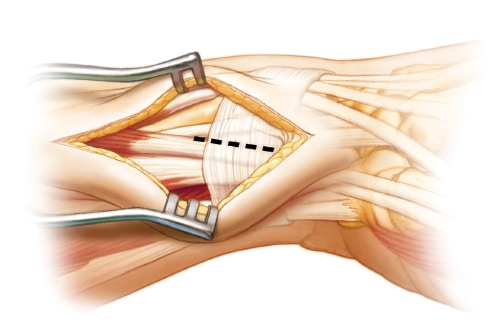
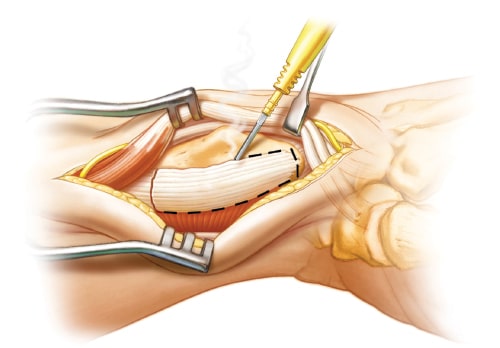
Brachioradialis Release
Release or excision of the insertion of the Brachioradialis (BR) tendon is required to provide adequate exposure of the radius and to remove one of the deforming forces. This action also releases the Pronator Quadratus muscle from its radial attachment. Identify and avoid the radial artery that is traveling parallel and palmar to the BR tendon.
Plate Placement
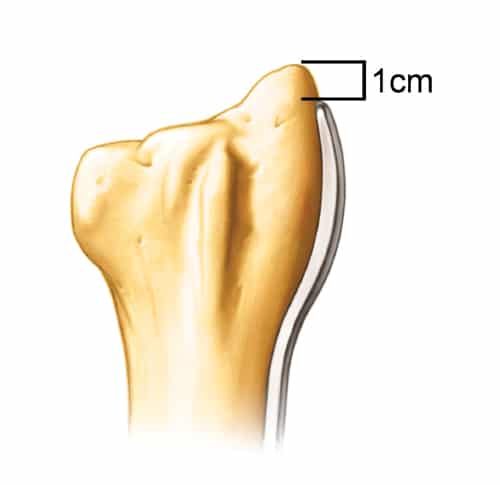
The tip of the radial styloid (RS) process is outlined with a bovie to help with the correct placement of the radial plate. This is one of the most important steps since this provides the anatomical reference for the correction of the malunion. The plate is placed approximately 1.0 cm proximal to the tip of the RS and midway between the dorsal and palmar surfaces. Intra-operative x-rays should be obtained at this time to assess the provisional position of the plate.
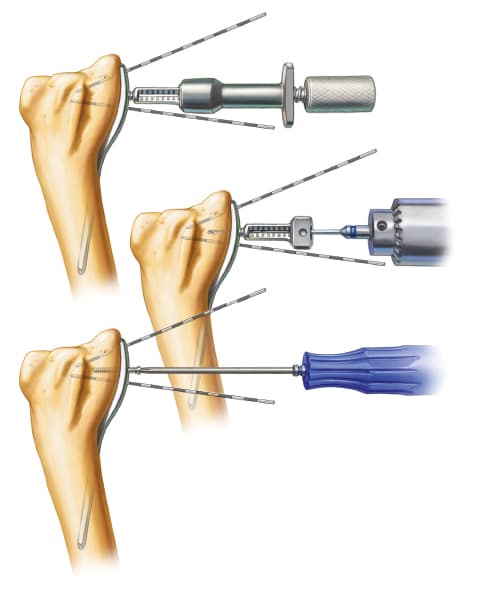
Distal Fixation
Once the correct distal position of the plate is determined, distal fixation of the plate is performed with 3 locking screws. Care is taken not to place any screws into the radial sigmoid notch. Note that the notch has a concave surface which may make this difficult to evaluate intra-operatively.
Making the Osteotomy
The osteotomy site is determined using the plate for the orientation of the cut. It should be 90 degrees to the distal segment of the plate, which starts between the 3rd and 4th hole. The 2nd and 3rd screws are temporarily removed and the 1st screw is loosened to allow for access to the osteotomy site without plate interference.
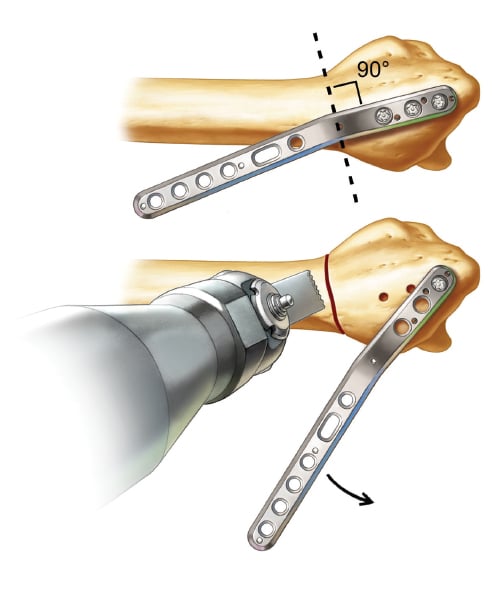
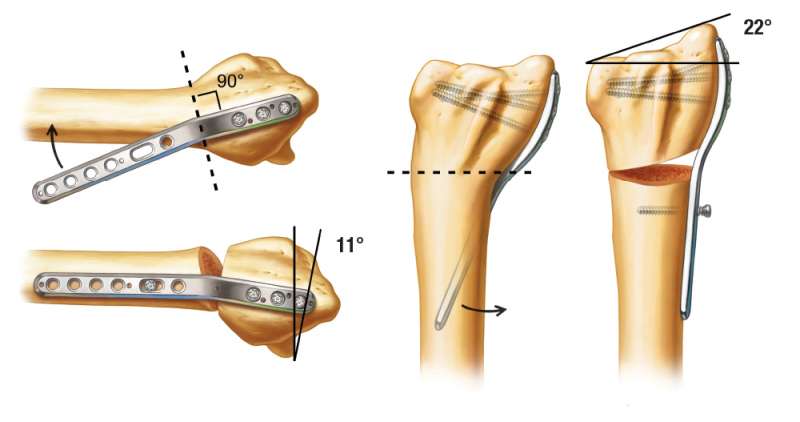
Reduction
The distal locking screws are reinserted. Reducing the proximal plate to the radial shaft performs the malunion correction. The correction obtained is 11 degrees of palmar tilt and 22 degrees of radial inclination.
Note: With severe deformities, the excess dorsal bone may need to be removed with a saw.
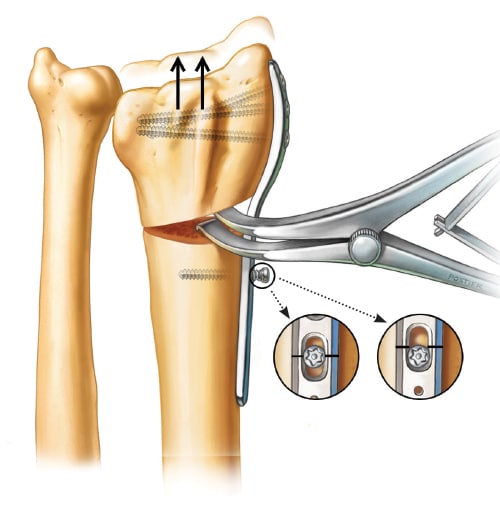
Regaining Length
The last step in correcting the malunion is to obtain the correct radial length. The laminar spreader can be used to achieve the appropriate length in severe shortening of the radius.
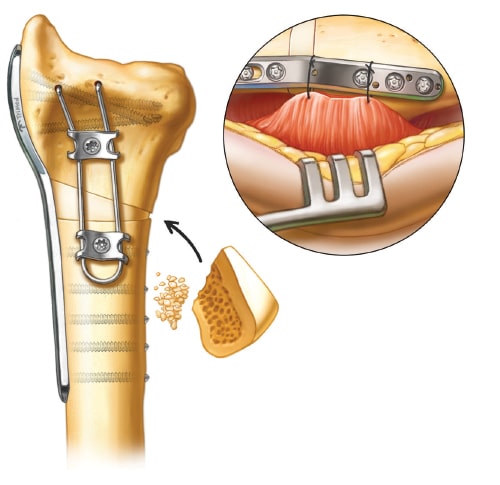
Supplemental Fixation and Bone Grafting
Supplemental fixation is obtained by placing a “wire-form” on the palmar side of the osteotomy, creating a “90-90” construct after a corticocancellous bone graft is inserted from the iliac crest (shape the graft to accommodate the defect). Reattachment of the PQ muscle can be performed by placing sutures through the empty holes on the radial plate.
Disclosure: The author did not receive any outside funding or grants in support of this work. Neither he nor a member of his immediate family received payments or other benefits or a commitment or agreement to provide such benefits from a commercial entity.